
Varicose veins of the lower extremities are often asymptomatic in humans. Often, the only problem with this pathology is the aesthetic defect in the legs caused by bulging superficial veins. In this case, the disease may be accompanied by pain or increased sensitivity of the skin of the feet. Depending on the severity of the disease, the patient is offered non-drug, drug or surgical treatment. Read more about the first symptoms of varicose veins, the nature of its course and effective methods of treatment and prevention, read our material.
What is it
Varicose veins are a pathology that only people suffer from. Animals do not have this problem, suggesting that the disease is associated with upright posture. When the person got to his feet, the main part of the circulating blood began to be below the level of the heart. In this case, all the conditions are created for the blood to circulate worse in the opposite direction, which leads to stagnation.
According to statistics, some disorders of the venous system have been observed in 80% of people in developed countries. Moreover, similar problems are increasingly found in young people. Apparently, one of the reasons why varicose veins are "rejuvenating" is a sedentary lifestyle, which only contributes to stagnation.
It is interesting that in the age group under 20, varicose veins of the lower extremities occur with the same frequency in both men and women. However, after the age of 20, women begin to dominate the structure of morbidity. This is due to pregnancy and childbirth, which are a serious factor in the development of venous diseases.
Properties, causes and mechanism of varicose vein development

The exact reasons for the formation of varicose veins of the lower extremities are still unknown. It is currently believed that the disease is caused by congenital or acquired defects of the valvular apparatus of the veins of the lower extremities.
A well-coordinated work of the venous valves is necessary for the unimpeded ascending flow of blood through the veins. These valves open only for blood flowing upwards. However, with a valve defect, partial descending blood flow is also possible. This is how venous insufficiency occurs, which is manifested by edema, leg muscle spasms and dilation of venous vessels.
Leukocytes may also be involved in the pathogenesis of varicose vein development. This issue is now being actively studied. It is assumed that with a prolonged accumulation of leukocytes in the tissues of blood vessels (especially in the area of the valve apparatus), an inflammatory process develops that spreads along the venous bed.
Because venous valves are subject to constant mechanical stress, inflammation develops particularly rapidly in the area of the venous valve apparatus.
Now the vast majority of people in developed countries lead a sedentary lifestyle. But then why doesn’t everyone have varicose veins? Consider the main risk factors that contribute to the development of this pathology:
- Hereditary factors. . . Despite the fact that the specific hereditary mechanisms associated with the development of varicose veins have not yet been established, most experts agree on the presence of such a factor. At the same time, there are strong counter-arguments regarding heredity in the development of varicose veins. For example, this is the prevalence of varicose veins among ethnic Africans and African immigrants who have gone to live in the United States. If the prevalence of varicose veins among sedentary Africans is about 0. 5%, then among immigrants this figure reaches 20%. These figures show that hereditary factors, at least, are not the only ones in the development of the disease and, most likely, do not predominate.
- obesity. . . Obese and obese people are at risk. It is important to note that obesity contributes to the formation of varicose veins both due to the increased load on blood vessels, and in connection with the risk of other diseases that affect blood vessels (diabetes mellitus, hypertension, etc. ).
- Pregnancy. . . This is one of the most obvious factors in the development of varicose veins of the lower extremities. In this case, the main risk factors are an increase in the volume of circulating blood, as well as compression of the retroperitoneal veins by the developing fetus in the uterus. According to epidemiological studies, second and subsequent pregnancies lead to a significant increase in the likelihood of developing varicose veins. After the first pregnancy, the probability of varicose veins on the legs remains small.
- Hormonal imbalance. . . Hormones are involved in the pathogenesis of most diseases. These pathologies include varicose veins. This problem is especially true for women who take hormonal contraceptives, as well as those who use hormone replacement therapy to treat certain diseases (e. g. osteoporosis) or during premenopause. Female sex hormones (especially estrogens and progesterone) have been found to reduce vascular tone and destroy collagen fibers. Thus, the vein wall is pathologically dilated.
- Lifestyle. . . A person's lifestyle has a great influence on the course of the disease. A sedentary lifestyle, as well as work related to prolonged standing or sitting (for example, security guards, drivers, office workers, service workers and others) contribute to the formation of varicose veins. You should also pay attention to your diet. Lack of sufficient amount of vegetables and fruits in the diet worsens the condition of the walls of blood vessels.
Stages of varicose veins of the lower extremities
Several classifications of varicose veins of the lower extremities are currently used. The international classification CEAP, adopted in 1994, is considered generally accepted. CEAP is an abbreviation, where each letter corresponds to the name of the classification category:
- C (clinical)- clinical class of the disease (type of affected veins, presence of pigmentation, eczema, trophic ulcers).
- E (etiological)- etiology of the disease (congenital, primary, secondary).
- A (anatomical)- anatomical localization of pathology (superficial or perforating veins).
- P (pathophysiological)- type of disorder (venous reflux, obstruction or a combination of both).
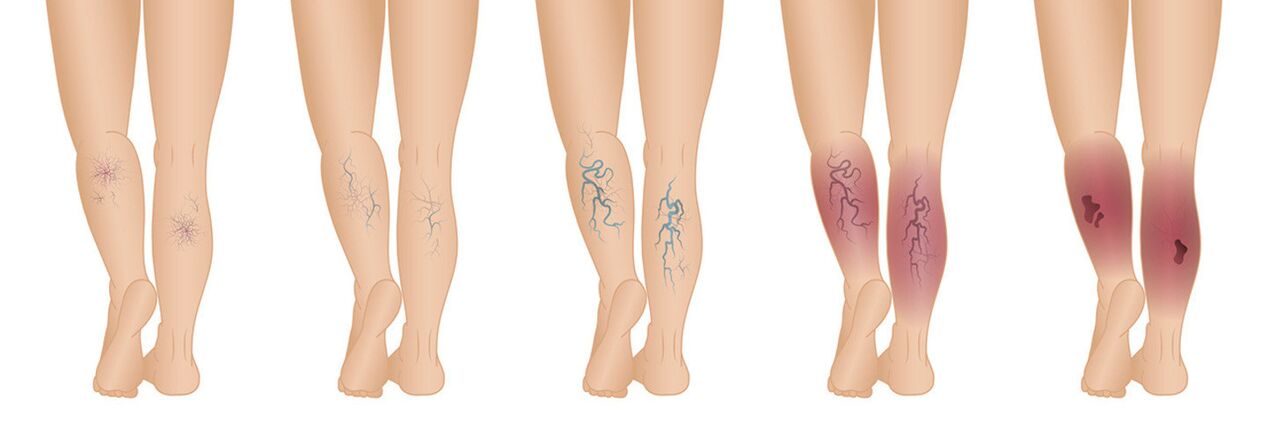
The course of the disease takes place in six stages:
- Zero stage. . . The earliest stage of varicose veins, in which even doctors cannot reliably diagnose. There are no external signs of the disease at this stage. Ultrasound diagnosis does not show the presence of pathology. At the same time, a person in the zero stage is concerned about symptoms such as swelling, a feeling of heaviness in the legs, as well as cramps, which indicates the presence of problems with blood vessels.
- The first phase. . . Already in the first stage of the disease, spider veins are visible on the surface of the skin of the feet, whose diameter is less than 1 millimeter. Medium-sized veins can increase in diameter up to 3 mm. At this stage, doctors are not always able to establish a correct diagnosis, because the presence of such asterisks does not always indicate varicose veins.
- Second phase. . . At this stage, the veins can appear and disappear depending on the conditions. For example, veins show up clearly after prolonged sitting, standing, or lifting heavy objects. The diameter of varicose veins at this stage is 3 mm or more. Blood clots often form in the second stage.
- The third phase. . . If the swelling of the legs appeared and disappeared in the previous stages of the disease, then in the third phase the edema becomes permanent. The swelling of the legs is strongest in the evening.
- The fourth phase. . . Significant trophic changes occur at this stage. The nutrition of the tissues near the affected veins is especially disturbed. The patient develops skin changes such as lipodermatosclerosis (inflammation of the subcutaneous fat tissue), eczema, as well as darkening or discoloration of the skin. The fourth stage of the disease is characterized by pigment changes. For example, the skin in the area of the affected veins may become brown and even black, indicating a concentration of pigments in this area. The opposite situation is also possible, when due to the pathological process the pigment does not enter the affected area, which leads to the appearance of pale skin. If varicose veins are not treated at this stage, the problem will only get worse with the further appearance of trophic ulcers.
- Fifth phase. . . At this stage of the disease, in addition to the above symptoms, trophic ulcers appear and heal quickly. If you do not take any treatment measures, then the ulcers will reappear again and again.
- Sixth phase. . . Trophic ulcers that do not heal appear. The temperature in the affected area increases significantly, and pus can leak from the wounds.
You should not wait for the development of the last stage - you should go to the doctor for another to register and monitor the dynamics of the disease. Sometimes the symptoms improve on their own, and sometimes they progress quickly. It is therefore important to monitor the situation in order to take action in time.
Symptoms

Consider the main symptoms of varicose veins of the lower extremities in different stages of the disease:
- Pain. . . This is the earliest sign of the disease. Since pain is a non-specific symptom, it is impossible to make a diagnosis based on this symptom alone. In varicose veins of the lower extremities, the pain is often localized along the venous trees.
- Feet in legs. . . It also refers to early symptoms, while the veins on the skin are not yet visible. Often the feeling of heat is accompanied by throbbing pain.
- Muscle cramps and itching. . . He usually gets upset at night.
- Swelling of the legs. . . In the early stages of the disease, the swelling is slight and transient. As a rule, they appear in the evening and disappear in the morning. However, as the disease progresses, the weight increases and they become permanent.
- Skin discoloration. . . As a rule, with varicose veins, the skin of the lower extremities darkens. In the area of the affected veins, the skin becomes brown. Eczema and dermatitis occur in the advanced stage of the disease. The final stages of varicose veins are characterized by the appearance of trophic ulcers. Initially, these are ulcers that heal, but later sores form that do not heal.
- Vascular spiders. . . In the medical literature, such asterisks are called telangiectasias. In some people, varicose veins may be confined to spider veins, without progression to larger veins.
- Distorted varicose veins. . . The most characteristic sign of varicose veins are twisted varicose veins on the surface of the legs.
In summer, the symptoms of varicose veins become more pronounced. This is due to the high ambient temperature, which already contributes to the spread of veins. Therefore, in the warmest hours, from 10 am to 4 pm, it is best to be in a well-ventilated area.
When to see a doctor
At the first symptoms of the disease - pain, swelling or the appearance of arachnids, you should consult a doctor. Because early-stage varicose veins are difficult to diagnose, they can be misdiagnosed at first. The patient should carefully monitor the condition of the legs and be monitored regularly by a phlebologist.
Diagnosis
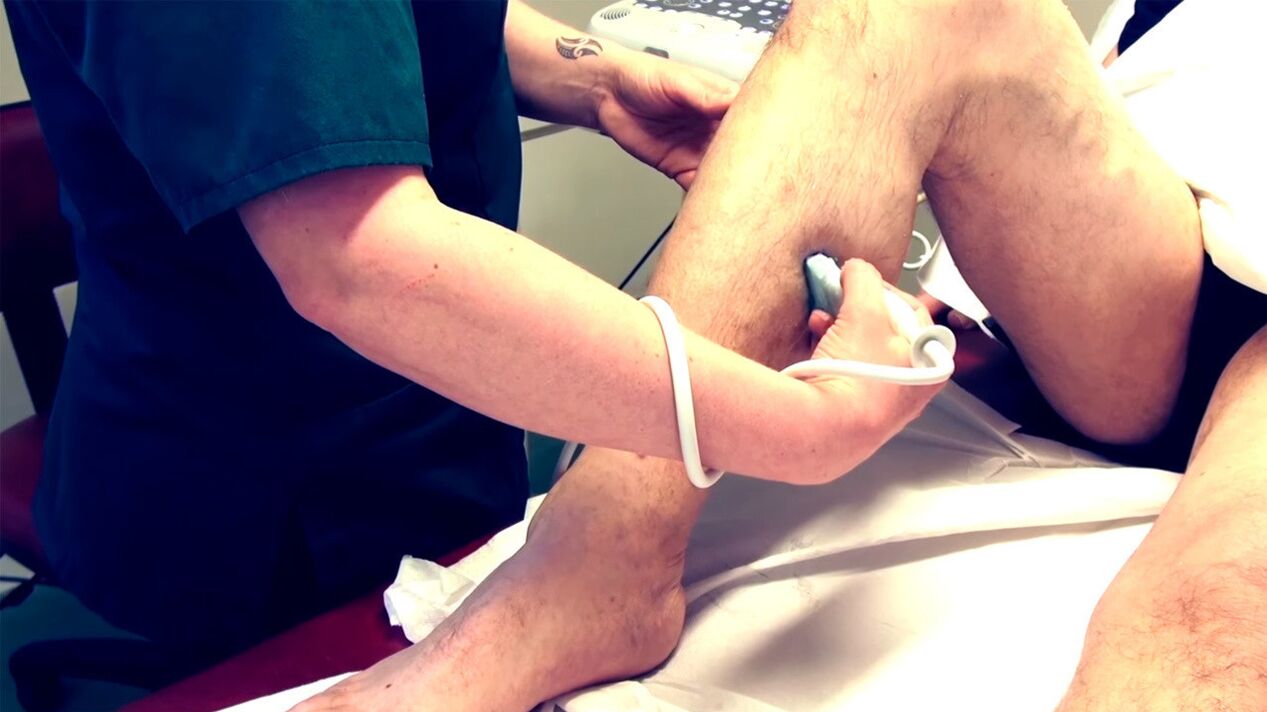
The diagnosis of varicose veins of the lower extremities comes down to the following activities:
- External examination of the skin of the feet;
- Doppler ultrasound;
- Duplex vein scanning;
- Phlebography.
Treatment characteristics
Varicose veins of the lower extremities are treated with both conservative and surgical methods. Conservative treatment is reduced to the following activities:
- Drug therapy. . . It is the intake of drugs that improve the tone of the venous walls. Also, the patient is prescribed drugs that reduce capillary permeability and improve blood microcirculation. If there is a risk of blood clots, then anticoagulants are prescribed.
- Compression therapy. . . It is wearing special compression socks, which reduce the load on the leg. The advantage is that it is possible to distribute the load evenly, even with heavy physical effort. When using a compression suit, congestion and swelling can be avoided.
- Corrective gymnastics and lifestyle changes. . . The patient is advised to exercise to reduce tension in the legs. It is important to avoid prolonged sitting or standing. If you have to stand or sit for a long time at work, then you need to take breaks more often.
If conservative therapy of varicose veins does not bring the expected results, then surgery is decided. These are most often minimally invasive interventions, including:
- Sclerotherapy- introduction into the vein of a substance that adheres to the walls of the affected vessel. This treatment leads to resorption of the arachnoid veins.
- Laser coagulation- introduction of a laser fiber into a vein and radiation of the walls with a laser, which also leads to sticking of the walls and further resorption of the blood vessel.
- Radiofrequency ablation- gluing veins with high frequency current.
- Phlebectomy- Removal of affected veins, in which blood circulation is worsened by 90%.
In some countries, you can have the operation for free, with compulsory health insurance. But it is not a fact that all types of compulsory insurance business are provided everywhere. In any case, help will be provided, but it is necessary to find out whether it will be conventional removal or laser.
Contraindications for people with varicose veins
- Sedentary lifestyle. . . It is important to avoid prolonged sitting or standing. Physical activity will help avoid congestion in the veins.
- Running and vigorous exercise. . . It is important not to overdo it with physical activity. If you have varicose veins, walking is definitely better than running.
- Unbalanced and unhealthy diet. . . You need to give up unhealthy foods, even if your health seems to allow. You should limit your intake of sweets, semi-finished products, as well as rich meat soups and smoked meats. But eating more vegetables and fruits would be a good idea.
- Hot tubs and showers. . . For people with vascular problems in the extremities, procedures with excessively hot and prolonged water are contraindicated.
Complications of varicose veins
Varicose veins can be complicated by trophic ulcers, phlebitis (inflammation of the veins) and deep vein thrombosis. The latter is the formation of blood clots in deep veins that threaten human life.
Conclusion
Symptoms of varicose veins of the lower extremities usually do not appear immediately. Different people have different sets of manifestations. For example, sometimes in this pathology there is no edema or no local increase in temperature or pain. This does not mean that there is no disease. A timely visit to the doctor will significantly slow the progression of the disease or even stop it, preventing the development of trophic changes.























